You might think heartburn is just an uncomfortable nuisance, but chronic acid reflux does lasting damage to your esophagus. When you ignore persistent symptoms, the lining of your tube to the stomach can actually transform. This transformation leads to a condition doctors call Barrett's Esophagus. It is a precancerous state that requires attention because, while rare, it can progress to serious illness.
We need to understand exactly what happens to the body before we discuss testing or treatment. Most people assume that if they take pills and feel better, the problem is gone. That assumption puts many patients at risk. Here is the reality of living with long-term acid issues and how modern medicine helps manage the hidden dangers.
The Transformation Behind Barrett's Esophagus
Barrett's Esophagus is a condition where normal squamous cells in the esophagus are replaced by specialized columnar epithelium resembling intestinal lining. Your esophagus is built to handle dry food moving down, not boiling acid backing up from your stomach. When you suffer from Gastroesophageal Reflux Disease, gastric acid sits on that lining for hours or days every week. Over time, usually more than ten years, the normal skin-like cells give up and swap out for tougher, acid-resistant cells similar to the intestine.
This cellular swap is called metaplasia. It sounds technical, but think of it as a survival mechanism gone wrong. The cells adapt to survive the acid bath, but these new cells carry a higher risk of mutating into cancer. Research indicates approximately 5.6% of the general population develops this condition. However, if you have confirmed chronic acid reflux, your risk jumps significantly to 10-15%. The scary part is that this change happens silently. You likely won't feel your cells changing types.
Understanding the Cancer Connection
Many people panic when they hear "precancerous." It is important to stay grounded with numbers. While Barrett's Esophagus is the primary pathway to Esophageal Adenocarcinoma, the progression rate is actually quite low for most individuals. Statistics show only about 5% of patients with Barrett's will ever develop esophageal cancer over their lifetime. However, the outcome for those who do is severe, with less than 20% surviving beyond five years after symptoms start.
Risk stratification tells us who needs to worry most. If you experience reflux symptoms more than three times a week for over 20 years, your risk of adenocarcinoma increases fortyfold compared to the average person. Demographic patterns are stark. The condition occurs three times more frequently in males than females. White men with obesity and a smoking history represent the highest-risk group. Understanding your personal profile helps determine if you fall into a category needing closer watching.
| Risk Factor | Impact Description |
|---|---|
| Chronic GERD Duration | Symptoms lasting more than 5 to 10 years increase likelihood |
| Male Gender | Men account for 79% of diagnoses despite population demographics |
| Obesity | BMI over 25 creates pressure increasing acid exposure |
| Smoking History | Tobacco use reduces saliva production and weakens lower sphincter tone |
| Age | Most commonly diagnosed in individuals older than 50 years |
Detecting the Condition Before Damage Spreads
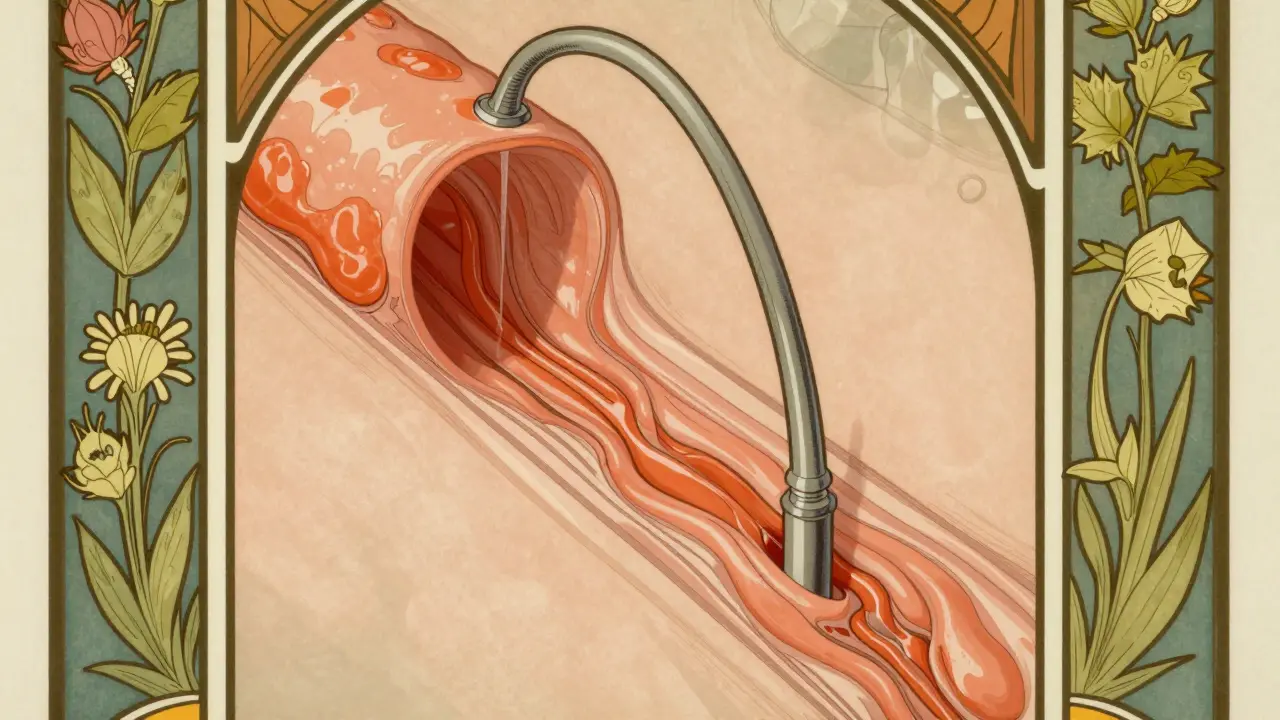
Because Barrett's Esophagus produces no specific symptoms, you cannot rely on how you feel. You could be burning with inflammation deep inside while feeling fine. The diagnostic gold standard remains upper endoscopy. During this procedure, a doctor slides a camera down your throat to look for "salmon-colored mucosa." Normal esophageal tissue looks pale pink or white. Barrett's tissue appears reddish-orange, distinct from the surrounding area.
Visual confirmation is just step one. Doctors must verify the cell type under a microscope. This means taking tissue samples. The standard method is known as the Seattle protocol. It requires collecting four biopsy samples every centimeter along the affected segment. This rigorous approach generates 12 to 24 samples per session. The goal is to catch focal dysplasia-early warning signs of bad cell behavior-that a single quick sample might miss.

Surveillance Schedules and Screening Rules
Screening isn't right for everyone due to cost-effectiveness and low prevalence in certain groups. Current consensus suggests targeting men over 50 with chronic reflux and other risk factors like smoking or family history. Women and lower-risk men generally do not warrant invasive screening unless other red flags appear.
Once diagnosed, surveillance becomes a schedule. Non-dysplastic Barrett's Esophagus usually needs an endoscopy every 3 to 5 years. If doctors spot Low-Grade Dysplasia, the clock speeds up to every 6 to 12 months. High-grade dysplasia is treated differently; you typically move toward active intervention rather than waiting.
New technologies are emerging to help reduce unnecessary scopes. Molecular biomarkers are currently being studied to identify which patients have the highest risk. Recent studies funded through 2026 aim to validate DNA methylation markers that could slash unnecessary surveillance endoscopies by 40%. Until these tools become routine, sticking to the interval plan prescribed by your gastroenterologist is vital.
Managing Acid and Reversing Changes
Management works on two fronts: stopping the damage and removing damaged tissue. For most, aggressive acid control is the foundation. Patients often prescribe themselves proton pump inhibitors based on comfort, but studies show conventional dosing may fail to fully suppress acid. Experts recommend high-dose regimens, such as omeprazole 40mg twice daily, to ensure complete suppression rather than just symptom relief.
Medication alone doesn't fix the tissue change. If dysplasia appears, endoscopic therapy steps in. Radiofrequency Ablation (RFA) has become the standard since 2010. It uses heat energy to destroy abnormal cells so healthy ones grow back. Trials like AIMS-2 showed 94% durable eradication of low-grade dysplasia with this method. Cryotherapy is another option used in complex cases.
Lifestyle plays a massive role too. Eliminating fatty foods, chocolate, and caffeine reduces reflux volume. Maintaining a BMI below 25 takes mechanical pressure off your stomach. Avoid eating within 3 hours of bedtime stops nighttime acid attacks. Elevating the head of your bed by 6 to 8 inches uses gravity to keep acid down. These steps complement medical treatment effectively.
Can Barrett's Esophagus go away on its own?
The condition rarely reverses completely without intervention. Once the lining changes to intestinal metaplasia, aggressive acid suppression and ablation therapies are required to remove the altered tissue and promote healing of normal lining.
How often should I get screened for Barrett's?
Frequency depends on severity. Non-dysplastic cases need checking every 3 to 5 years. Low-grade dysplasia moves to every 6 to 12 months. High-grade dysplasia usually prompts immediate treatment rather than monitoring.
Is there a blood test for Barrett's Esophagus?
Currently, endoscopy with biopsy is the only definitive way to diagnose it. Blood tests cannot detect the cellular changes in the esophagus, though research into molecular saliva assays is ongoing.
Does losing weight help reverse Barrett's?
Weight loss significantly reduces acid reflux episodes and pressure on the lower esophageal sphincter. While this prevents further damage, established intestinal metaplasia usually requires medical removal to restore normal tissue.
What symptoms signal the need for an endoscopy?
Difficulty swallowing solid foods, pain radiating to the chest, or heartburn occurring weekly for years are major signals. Even without visible symptoms, long-term male patients with obesity should discuss screening options with a specialist.

Molly O'Donnell 31.03.2026
This information is absolutely terrifying when you realize how silent the damage truly is.
Rocky Pabillore 31.03.2026
Most laypeople simply cannot grasp the nuance of gastrointestinal pathology without proper academic training in gastroenterology.
The average person ignores warning signs until irreversible cellular damage has already occurred within their physiology.
True understanding requires reading peer-reviewed literature rather than relying on anecdotal forum discussions about symptoms.
One must approach this subject with the rigor of a clinical researcher instead of casual curiosity.
Superior knowledge dictates that screening protocols be followed strictly by those who actually comprehend the risks involved.
Rod Farren 31.03.2026
The pathophysiology of Barrett's esophagus involves metaplastic transformation of the distal squamous epithelium to columnar epithelium.
This process occurs secondary to chronic acid exposure and bile reflux injury.
Proton pump inhibitors remain the cornerstone of management strategies for symptom suppression.
However, complete mucosal healing is often elusive despite maximal medical therapy.
Endoscopic surveillance is mandated for patients with confirmed intestinal metaplasia.
The Seattle biopsy protocol dictates four quadrants per centimeter of visible segment.
High-definition chromoendoscopy enhances lesion detection rates significantly during endoscopy.
Radiofrequency ablation offers durable eradication of dysplastic tissue effectively.
Cryotherapy serves as an alternative adjunct for refractory cases involving stricture formation.
Molecular biomarkers represent the frontier of non-invasive risk stratification methods currently under investigation.
DNA methylation patterns correlate strongly with malignant progression potential in longitudinal studies.
Surveillance intervals are contingent upon histologic grade of dysplasia present upon sampling.
Low-grade dysplasia necessitates endoscopy every six months for optimal monitoring outcomes.
Ablation therapy prevents progression to invasive adenocarcinoma in the vast majority of patients.
Patients must understand that lifestyle modifications alone rarely reverse established metaplasia permanently.
Russel Sarong 31.03.2026
Oh wow!....this is SO much info!!
And I agree.. completely!!!
The risk factors.. are definitely real!!!
We need to wake up... NOW!!!
...Everyone listening... should prioritize their gut health!!!
...Don't wait!!!...
Christopher Beeson 31.03.2026
Society ignores the slow murder of the esophagus while prioritizing superficial aesthetics and trivial comforts.
You walk around swallowing poison daily and wonder why your body eventually collapses under the chemical assault.
The modern lifestyle is essentially a death sentence wrapped in convenience food and late-night snacking rituals.
People claim ignorance about health risks yet demand miraculous cures when the biological system finally fails.
Truth is uncomfortable when staring down the barrel of cellular degeneration caused by negligence.
Everyone is complicit in their own decline by refusing to confront the visceral reality of chronic inflammation.
Fear drives action yet denial paralyzes millions into accepting permanent damage as normalcy.
You will never heal if you do not accept the severity of your metabolic and structural vulnerabilities today.
Sharon Munger 31.03.2026
thanks for posting this its helpful info for sure.
i had a relative go through this years ago and it was tough dealing with the scopes.
glad to see updated stats on risk factors for men especially.
hope everyone takes care of themselves.
Owen Barnes 31.03.2026
its realy hard to stay on top of all this stuff when life gets busy and you forget your meds.
i think most of us could do better with eating habits and weight loss plans too.
doctors say its important but we dont always listen until something hurts badly.
hope evryone here stays safe and knows when to call for help early.
dont ignore the burning feeling in your chest area anymore.
Cara Duncan 31.03.2026
I really appreciate everyone sharing their experiences here because health topics can feel so isolating sometimes 😌🫂.
It is nice to see people supporting one another through these diagnoses without fear mongering.
We should all take care of our bodies and listen to what they are telling us daily. 🩺💊
Don't forget that prevention starts with small changes like diet and sleep posture. 💤🍎
Sending good vibes to anyone navigating a new diagnosis right now! ✨❤️
Jenny Gardner 31.03.2026
The statistical data presented regarding gender disparity in diagnosis is particularly noteworthy.
Men constitute a significantly larger proportion of the affected demographic compared to women.
Obesity correlates strongly with the mechanical pressure exerted upon the lower esophageal sphincter.
Tobacco use diminishes protective mechanisms such as salivary neutralization capacity.
Regular surveillance remains essential for those falling within the high-risk cohort classification.