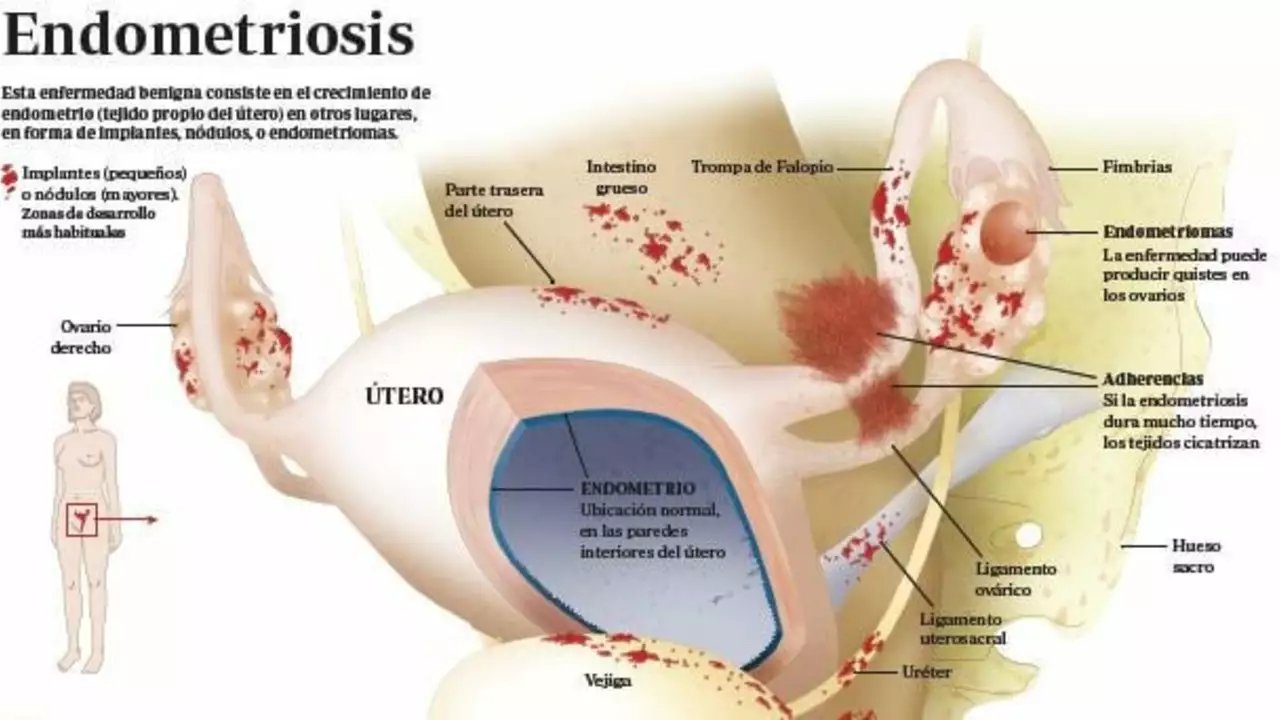
Endometriosis: Practical Guide to Symptoms, Diagnosis and Treatment
Endometriosis is a condition where tissue similar to the lining of the uterus grows outside the uterus. It causes pelvic pain, heavy periods, pain during sex, and sometimes fertility problems. Symptoms vary—some people have mild discomfort, others have constant pain that gets worse during periods. Knowing the common signs helps you get care sooner.
Pain can be sharp, cramping, or a dull ache in the lower belly, back, or hips. Bowel or bladder pain, especially around your period, is common when endometrial-like tissue is near those organs. Fatigue and bloating often show up too. If you notice painful periods that get in the way of work, school, or sleep, bring it up with your doctor.
Diagnosis starts with a clear history and pelvic exam. Doctors use ultrasound to look for cysts called endometriomas, but small implants often don’t show up on imaging. Laparoscopy, a minor surgical procedure, is the gold standard because it lets doctors see and possibly remove lesions. If surgery isn’t an option, doctors may make a working diagnosis based on symptoms and response to treatment.
Treatments aim to ease pain and protect fertility. Over-the-counter pain relievers like ibuprofen can help short-term. Hormonal options—combined birth control pills, progestins, and GnRH agonists or antagonists—reduce or stop ovulation and can shrink lesions. Each option has trade-offs: some cause mood changes, bone density loss, or hot flashes. Talk to your provider about what fits your goals, especially if you want to get pregnant.
Surgery can remove scar tissue and cysts and often improves pain and fertility when done by a skilled surgeon. Conservative surgery preserves the uterus and ovaries; in severe cases, hysterectomy might be discussed, but only when other options fail and fertility is not desired. Ask about referral to a specialist experienced in endometriosis surgery.
Lifestyle steps can make daily life better. Regular moderate exercise eases pelvic pain for many people by reducing inflammation and improving mood. Heat packs, pelvic floor physiotherapy, and mindfulness or cognitive-behavioral therapy help manage chronic pain. Diet changes—reducing processed foods and alcohol—may help some, though results vary.
If you’re trying to conceive, fertility treatments like timed intercourse, intrauterine insemination, or IVF can help depending on age and disease severity. Early referral to a fertility specialist speeds up the right plan. Keep records of cycles, symptoms, and treatments—this makes appointments more productive.
When to see help now: severe pelvic pain, heavy bleeding that soaks a pad or tampon in an hour, fever with pelvic pain, or sudden worsening of symptoms. Don’t accept being told pain is “normal” if it disrupts your life.
Our site collects practical articles, drug guides, and how-to tips to help you navigate treatment choices and pharmacy options. Read patient-focused pieces, compare medications, and use our resources when talking with your clinician.
Join support groups or online forums to share tips and emotional support. Track pain, sleep, and medication side effects in a simple app to spot patterns and show your doctor clear data.