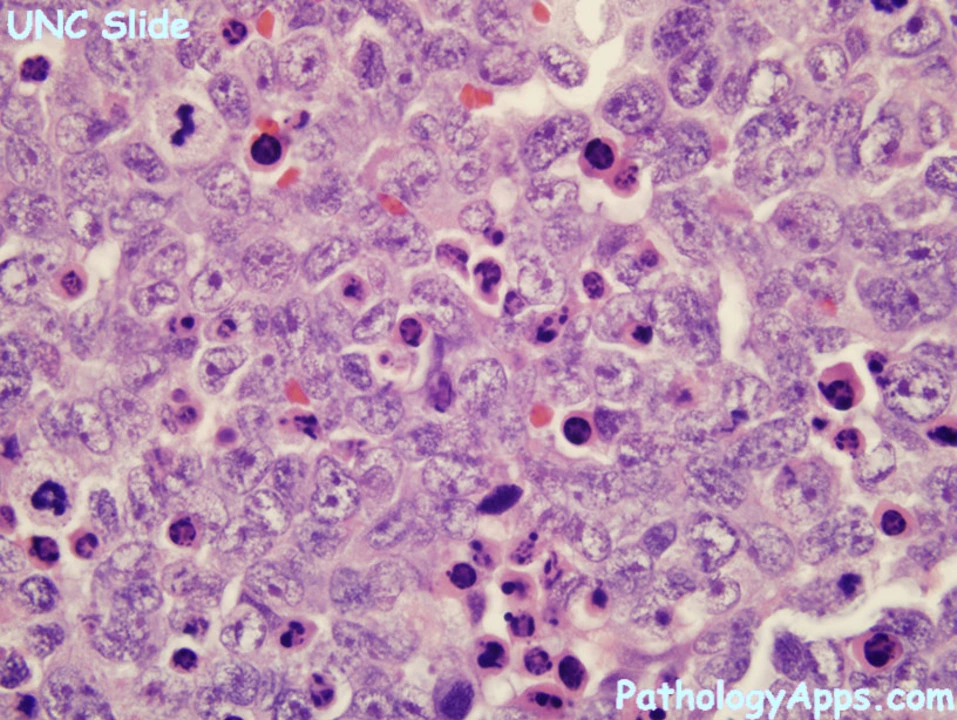
Rhabdomyosarcoma: What You Need to Know Right Now
Rhabdomyosarcoma (RMS) is a rare cancer that starts in muscle-like cells. It shows up most often in children but can affect adults too. If someone you care about has a fast-growing lump, new swelling, or unexplained bleeding, RMS is one of the things doctors check for—early action matters.
How it looks and where it shows up
RMS can appear almost anywhere. Common spots are the head and neck, the chest or abdomen, the genitals and urinary tract, and the arms or legs. Symptoms depend on location: a lump under the skin, trouble breathing, a blocked bladder, a persistent nosebleed, or vision changes. Pain isn’t always present, which is why new lumps should never be ignored.
There are a few main types: embryonal (more common in young kids), alveolar (tends to be more aggressive), and other rare subtypes. The exact type affects treatment choices and outlook.
How doctors find out
Diagnosis starts with a physical exam and imaging—usually ultrasound, CT, or MRI. Those tests show size and where the tumor is, but a biopsy is the only way to confirm RMS. Pathology will tell the subtype and features that guide therapy. Doctors also run tests to see if the cancer has spread—this may include a PET scan, bone marrow check, or additional imaging.
Treatment is often multi-step. Surgery removes as much tumor as possible. Chemotherapy is a key part of treatment for most patients—it targets cancer cells throughout the body. Radiation helps when surgery can’t remove everything or when the tumor is in a spot where surgery would cause major harm. Your team may combine these approaches based on age, tumor type, and stage.
Side effects are real but manageable. Chemotherapy can cause nausea, hair loss, and low blood counts. Radiation can damage nearby tissues and cause long-term effects, especially in growing children. That’s why treatment plans try to balance curing the disease and preserving quality of life.
Prognosis varies. Localized tumors treated early have much better outcomes than cancers already spread at diagnosis. Embryonal RMS generally has a better prognosis than alveolar RMS. Long-term follow-up matters: survivors need regular checkups for recurrence and late effects of treatment.
Practical tips: get a clear treatment plan in writing, ask about side-effect management and fertility preservation if relevant, and consider a second opinion at a pediatric or sarcoma center. Ask your doctor: What subtype is this? What stage? What are the goals of treatment? What support services are available?
No one faces this alone—look for specialists, support groups, and resources that focus on sarcoma and pediatric cancer. Quick and clear communication with your care team makes a big difference in both treatment and recovery.