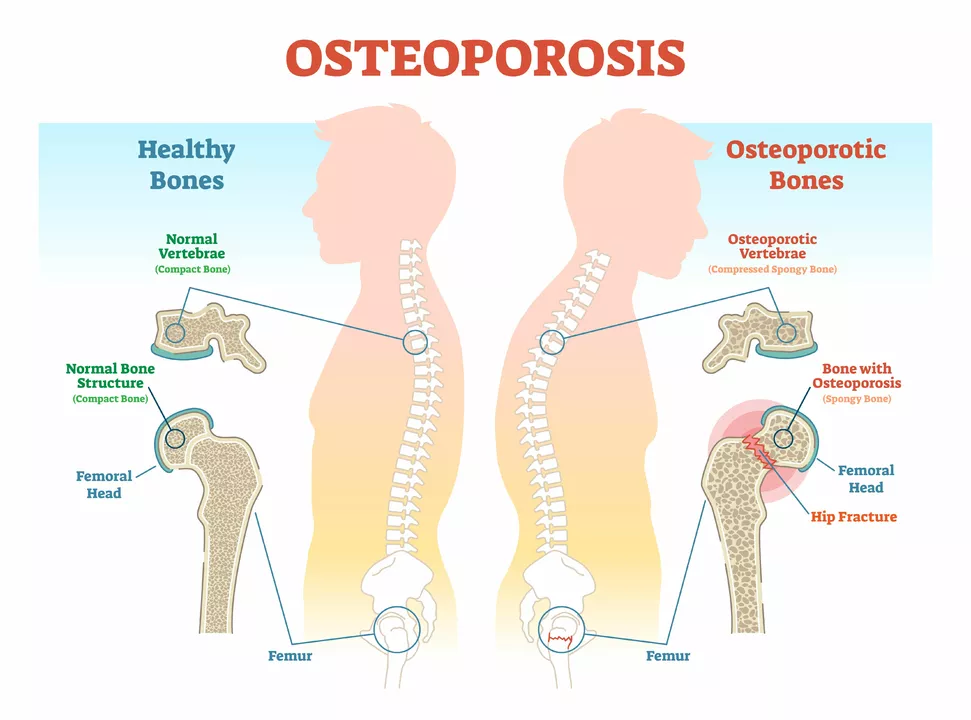
Osteoporotic fractures: how to prevent, spot, and treat
One broken hip often means months of rehab and a higher chance of losing independence. Osteoporotic fractures happen when bones are weak and break from a low-impact event — like a fall from standing height or a minor bump. The usual spots are the hip, spine and wrist. Knowing the risk factors and the simple steps you can take makes a big difference.
Risk factors are easy to check. Older age, female sex after menopause, past fractures, long-term steroid use, low body weight, smoking, heavy drinking and certain medical conditions raise your odds. If any of that sounds like you, bring it up with your doctor.
Screening is straightforward. Ask about a DEXA bone density scan to get a T-score and an idea of bone strength. Your doctor may also calculate a 10-year fracture risk (commonly called FRAX) and run basic blood tests to rule out treatable causes like low vitamin D or thyroid problems. These tests guide whether you need medication and what kind.
Preventing osteoporotic fractures
Start with three concrete habits. First, nutrition: aim for about 1,000–1,200 mg of calcium daily and 800–1,000 IU of vitamin D, unless your doctor says otherwise. Get calcium from dairy, fortified foods or supplements if needed. Second, exercise: do weight-bearing cardio (walk, jog, dance) most days and strength training twice a week. Add balance work — heel-to-toe walking or single-leg stands — to cut fall risk. Third, cut risky habits: stop smoking and keep alcohol moderate.
Home safety matters. Remove loose rugs, add grab bars in bathrooms, improve lighting, and wear shoes with good grip. Have your vision checked yearly and review medications with a clinician to reduce dizziness or falls. If you have frequent falls, ask about a physical therapy plan focused on balance and strength.
When lifestyle changes aren’t enough, medication helps. Common options include oral bisphosphonates (like alendronate), yearly IV treatments, and newer injections. These drugs can lower the chance of a hip or spine break, but they have pros and cons. Discuss side effects and how long you should stay on treatment with your provider.
What to do after a fracture
If you break a bone, get medical attention fast. Imaging will show the damage and guide treatment. Hip fractures often need surgery; many spinal fractures can be managed with pain control, bracing or procedures like kyphoplasty in select cases. Early mobilization and a rehab plan speed recovery and lower complications.
After the immediate problem is managed, treat the underlying bone weakness. That means a full bone-health review, starting or adjusting osteoporosis medicine if needed, and fixing any fall risks at home. Follow-up with a bone clinic or your primary care doctor keeps you on track and helps prevent another break.
Want one concrete next step? If you’re over 65, postmenopausal with risk factors, or you’ve had a prior fracture, ask your doctor for a DEXA scan. A quick test and a short conversation can change the road ahead for your bones.